Chronic Pain and Depression: Why Sleep Is the Hidden Link
Chronic pain—ongoing pain lasting more than 3 months—disrupts sleep, and poor sleep makes both pain and depression worse. If you’re lying awake at 3am because your back hurts, then dragging through the next day feeling hopeless, you’re caught in one of the most vicious cycles in medicine. Symptoms of depression and anxiety are present in 50% to 80% of people with chronic pain, and sleep problems, chronic pain, and depression are closely connected in what doctors call the “Sleep-Pain-Depression Triangle.”
How Does Chronic Pain Affect You Mentally?

Chronic pain doesn’t just hurt your body—it fundamentally changes how your brain processes stress, emotion, and sleep. The relationship between chronic pain and depression involves shared neurotransmitters and nerve pathways in the brain and spinal cord, which is why the two conditions so often occur together. Chronic pain can cause long-term changes in the brain’s structure and function, affecting areas involved in mood regulation and emotional processing.
When chronic pain keeps you awake night after night, the effects compound quickly. Chronic pain can disrupt sleep and cause fatigue during the day, leaving you exhausted, irritable, and unable to cope with normal stress. Many patients with chronic pain describe feeling like they’re functioning on empty—going through the motions but barely holding it together. The dopaminergic system of the midbrain is affected by chronic pain, which can damage dopamine activity and contribute to depressive disorders.
The mental health symptoms of chronic pain go beyond just feeling tired. Depression and anxiety become more likely as sleep deprivation accumulates. Research shows that approximately 40% of adults with chronic pain experience clinically significant depression and anxiety disorders. Studies indicate that 62.9-75% of chronic pain patients have at least one psychiatric disorder, with depression being the most common. The prevalence of major depressive disorder among adults with chronic pain is 36.7%, while generalized anxiety disorder affects 16.7% of patients with chronic pain. Women and younger adults are at higher risk for depression and anxiety when experiencing chronic pain.
The Social Cost of Sleep-Deprived Chronic Pain
Chronic pain often forces people to give up hobbies, work responsibilities, and social activities. In a transplant-heavy city like Charlotte, where many people are still building their social networks, the isolation can hit especially hard. When you’re too exhausted to meet friends at Sycamore after work, or you cancel plans because you haven’t slept in days, those connections fray quickly. Depression from chronic pain can also strain relationships with partners and family members who may not understand what you’re going through.
The Sleep-Pain-Depression Cycle: How It Works
This isn’t just “feeling tired”—it’s a biological feedback loop where each problem makes the others worse. Understanding this cycle can help you recognize why standard approaches like “just get more rest” don’t work.
Chronic pain disrupts sleep. Pain interferes with your ability to fall asleep and stay asleep. Studies show that chronic pain patients with sleep problems report greater pain severity and more disability.
Sleep deprivation amplifies pain sensitivity. When you don’t sleep well, your central nervous system becomes more reactive to pain signals. What might have been tolerable chronic pain when you’re rested becomes unbearable after a sleepless night. This affects all types of chronic pain conditions, from chronic low back pain to chronic headaches.
Poor sleep triggers depressive disorders. Sleep deprivation affects the same neurotransmitters involved in depression—serotonin and norepinephrine. Chronic stress changes brain chemistry, making you more vulnerable to major depressive disorder. Developing new sleep problems when you have chronic pain more than triples your risk of developing depression.
Depression worsens both pain and sleep. Depression increases pain sensitivity, making chronic pain feel more intense. Depression also disrupts sleep independently, creating insomnia even when pain is controlled. Research shows that good sleep can protect you from some negative effects of pain on mood—when patients with chronic pain get better sleep, the connection between their pain and depression becomes weaker.
In our Charlotte practice, we often see this pattern with banking and corporate professionals who’ve been pushing through chronic pain for months. By the time they reach us, they’re dealing with clinical depression triggered by sleep deprivation. Breaking any part of this cycle can help the whole system improve.
Why “Just Push Through” Makes It Worse
Many patients suffering from chronic pain try to maintain their normal schedule despite pain and exhaustion. In Charlotte’s achievement-oriented culture, there’s pressure to stay productive. But “pushing through” when you’re sleep-deprived actually reinforces the cycle. Your body never recovers, pain sensitivity increases, and depression and anxiety worsen.
When Chronic Pain Becomes Too Much
The tipping point often isn’t the pain itself—it’s when sleep deprivation makes you unable to function. You might reach a point where you’re having thoughts of hopelessness, struggling to get out of bed, or wondering if life is worth living. These are signs that chronic pain has triggered major depression and requires immediate attention.
Warning signs that chronic pain and depression need urgent treatment:
- Persistent thoughts of suicide or self-harm (call 988 for the Suicide & Crisis Lifeline)
- Unable to perform daily tasks like showering, eating, or working
- Severe depression lasting more than two weeks—deep sadness, loss of interest, feelings of worthlessness
- Pain worsening despite treatment, especially with new neurological symptoms
- Increasing social withdrawal—canceling plans, avoiding people
- Using substances to cope with pain or sleep
If you’re experiencing any of these, chronic pain has crossed from a physical problem into a mental health crisis. Both depression and chronic pain are treatable conditions—you don’t have to live this way.
Sleep Deprivation as a Breaking Point
For many people with chronic pain, the breaking point comes after weeks or months of fragmented sleep. The cumulative effect of never sleeping well eventually breaks down your ability to cope with depression and anxiety. This is your body and brain signaling they need help.
What Medication Is Used for Chronic Pain and Depression?
Certain antidepressants can reduce the perception of pain while also treating depression and anxiety. This isn’t about masking symptoms—these medications address shared biological mechanisms between chronic pain and depression. Talk with your doctor or psychiatrist about which options below might fit your situation. Medication decisions should be individualized based on your specific pain type, mental health symptoms, medical history, and other medications.
Common medication approaches include:
Tricyclic antidepressants like amitriptyline and nortriptyline are effective for forms of neuropathic pain, particularly diabetic neuropathy and chronic back pain. Tricyclic antidepressants can also improve sleep quality, which helps break the pain-depression cycle. These medications are often used in pain management strategies for chronic neuropathic pain conditions.
SNRIs (serotonin and norepinephrine reuptake inhibitors) such as duloxetine and venlafaxine work on both pain and depression pathways. These antidepressant medications can reduce pain intensity while treating depressive symptoms. SNRIs are particularly effective for chronic musculoskeletal pain, chronic low back pain, and neuropathic pain conditions like diabetic neuropathy.
SSRIs (selective serotonin reuptake inhibitors) like sertraline are primarily used for treating depression and anxiety disorders, though they’re less effective for pain than SNRIs or tricyclics. They may be appropriate when anxiety is a primary concern, particularly for patients with chronic pain who also have panic disorder or social anxiety disorder. SSRIs can help manage the psychological distress associated with ongoing pain.
Medications and psychotherapy can help relieve depression and make chronic pain more tolerable. A comprehensive treatment plan typically includes both—medications help stabilize brain chemistry, while therapy teaches skills to manage symptoms.
Medication Limitations
Pain medications alone rarely solve chronic pain. Antidepressant therapy helps many people but usually works best when combined with talk therapy, exercise, and sleep hygiene improvements. Think of medication as one tool in pain management, not the complete solution.
What Is the Best Psychological Treatment for Chronic Pain?
Cognitive-behavioral therapy (CBT) is the most well-studied psychological treatment for chronic pain and co-occurring depression. Multiple systematic review studies confirm that psychological therapies can reduce pain intensity, improve mood, and help you participate in meaningful activities again. Evidence-based psychological therapies address both the physical experience of chronic pain and the mental health symptoms of depression and anxiety.
Evidence-Based Therapy Approaches
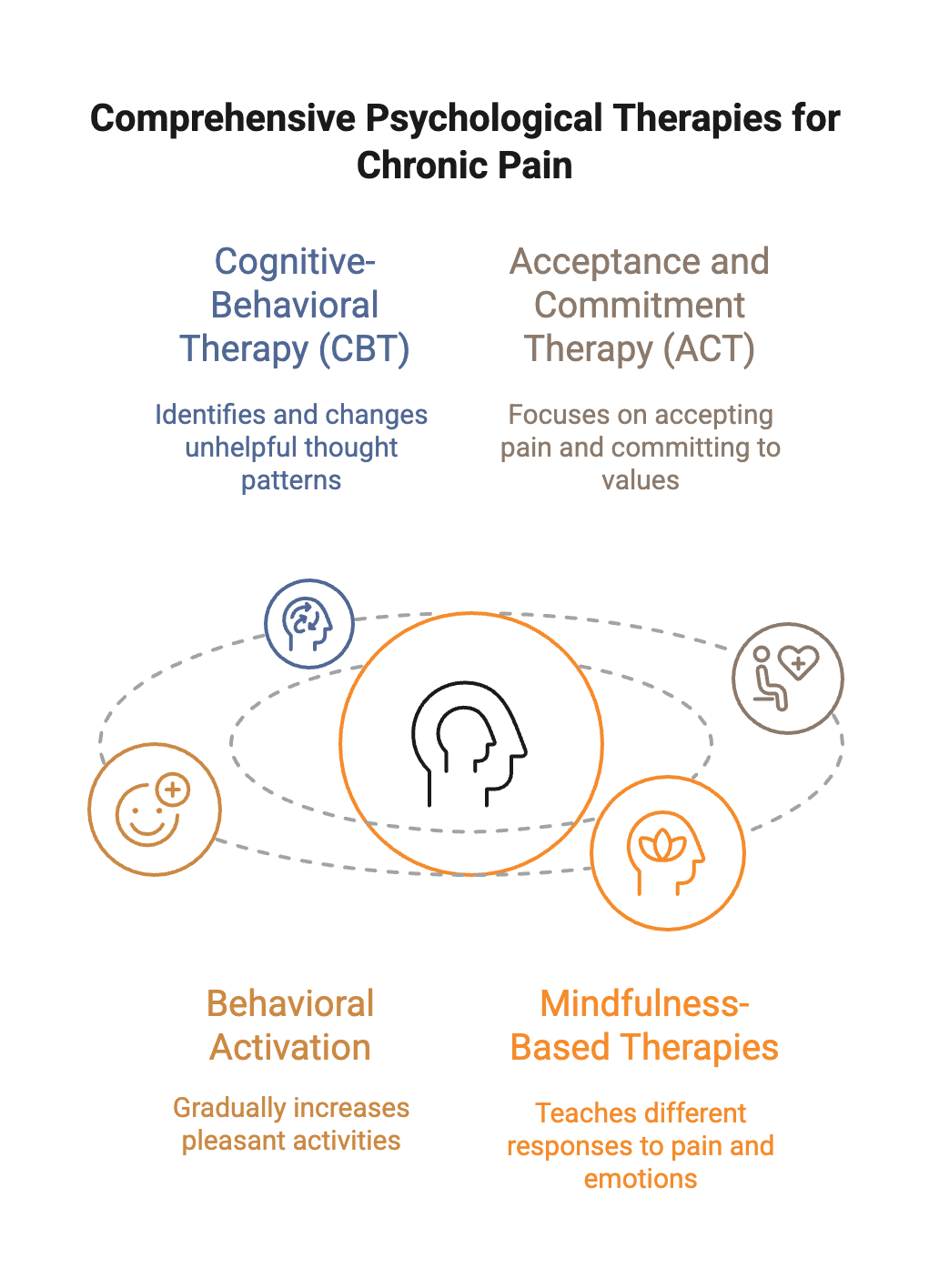
Cognitive-Behavioral Therapy (CBT) helps you identify and change unhelpful thought patterns that worsen chronic pain and depression. For sleep issues, Cognitive Behavioral Therapy for Insomnia (CBT-I) is one of the most effective treatments and can improve sleep quality while reducing depression and anxiety in patients with chronic pain.
Acceptance and Commitment Therapy (ACT) focuses on accepting chronic pain rather than fighting it, while helping you commit to actions aligned with your values. This approach is particularly helpful when sleep disruption has led to avoiding activities you care about.
Behavioral Activation gradually increases pleasant activities, even when you’re tired and in pain. This directly counters the withdrawal and isolation that depression and anxiety cause.
Mindfulness-Based Therapies teach you to respond differently to pain sensations and difficult emotions, and can improve sleep quality by reducing racing thoughts.
We frequently use CBT and behavioral activation with Charlotte clients dealing with chronic musculoskeletal pain and sleep problems. The goal isn’t eliminating chronic pain entirely—it’s helping you function better despite pain, which often leads to better sleep, which then reduces both pain and depression.
Why Therapy Works When You’re Exhausted
Therapy for chronic pain doesn’t require perfect energy. Sessions can be adjusted to your state, and techniques like sleep hygiene and activity pacing actually help you regain energy over time.
Other Helpful Approaches
Exercise can reduce chronic pain, boost mood, and improve sleep quality. Physical activity helps ease depression and anxiety by releasing brain chemicals similar to those affected by antidepressant medications.
Sleep hygiene and activity pacing strategies help you work with your body’s limits. Learning to pace activities and establish consistent sleep routines can reduce pain flares and improve rest.
Integrated care that addresses both mental and physical health is essential for treating chronic pain and depression. This means working with providers who understand that chronic pain and mental health conditions require coordinated treatment.
Getting Help for Chronic Pain and Depression in Charlotte
If you’re caught in the sleep-pain-depression cycle, the most important step is recognizing you don’t have to manage chronic pain and depression alone. Whether you’re a transplant professional still building your support network or someone who’s been dealing with chronic low back pain for years, specialized psychological treatment for chronic pain can help you break the cycle. Evidence-based approaches can address co-occurring depression and anxiety while helping you manage pain symptoms more effectively.
Ready to Get Started?
Our South End practice specializes in evidence-based psychological therapies.
Connect with our chronic pain specialists →
Common Questions About Chronic Pain and Depression
What Types of Chronic Pain Are Most Linked to Depression?
All forms of chronic pain can contribute to depression and anxiety. Chronic low back pain is one of the most common, frequently co-occurring with depression and anxiety. Chronic musculoskeletal pain conditions, including rheumatoid arthritis, show elevated depression rates. Neuropathic pain like diabetic neuropathy is especially challenging. Chronic headaches and migraine headaches also have high rates of co-occurring depression and anxiety.
How Do Clinical Symptoms Differ Between Acute Pain and Chronic Pain?
Acute pain is your body’s normal response to injury, typically resolving within weeks. Chronic pain persists beyond normal healing time—usually longer than 3 months. The clinical symptoms of chronic pain extend beyond physical discomfort. Patients with chronic pain often develop depression and anxiety including persistent sadness, loss of interest, irritability, and difficulty concentrating. The transition from acute pain to chronic pain often involves changes in how the brain and spinal cord process pain signals.
Can Treating Sleep Help Prevent Depression in People With Chronic Pain?
Yes, research shows that treating sleep problems may help prevent depression in patients with chronic pain. Developing new sleep problems when you have chronic pain more than triples your risk of developing major depressive disorder. Good sleep quality can protect you from negative effects of pain on mood. This is why many pain management programs now include sleep-focused interventions like CBT-I alongside treatment for chronic pain and depression.
This blog provides general information and discussions about mental health and related subjects. The content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
CTA Text Suggestions:
- Header: Ready to get started?
- Link Option A: Connect with our chronic pain specialists →
- Link Option B: See our pain and depression therapists →